 |
||||||||||||
|
March/April 2017
BY CLAUDIA GARY Although they created less drama than Dustoff, many other medical advances took place during the Vietnam War that helped save countless lives and limbs. These contributions to combat casualty care—and the physicians who implemented them—improved the outcomes for those wounded in Vietnam as compared to previous wars and have offered important ongoing contributions to military and civilian medicine. The rapid evacuation to treatment sites combined with other factors to create a situation that was more than the sum of its parts, especially when you add the dedication of team members. Those other essentials included state-of-the-art emergency response and trauma-care techniques, improved storage and distribution of blood resources, improvements in wound care and burn care, detailed assessments of the wounding capacity of different weapons, improved surgical methods, the proximity to the battlefield of small surgical hospitals, and the well-trained surgeons, anesthesiologists, nurses, and other staff who worked tirelessly. Military medicine is imbued with tradition. Some physicians and surgeons who served in Vietnam were inspired to do so by family members or teachers who had served in past wars. Since coming home, some have continued to contribute by helping to educate military physicians.
During the Vietnam War, “Topical antimicrobial chemotherapy for the care of burns and other wounds was for the first time available in the theater of operations,” said Dr. Rasmussen. “The current Department of Defense Center of Excellence Joint Trauma System Clinical Practice Guidelines recommend topical antimicrobial chemotherapy for burn wounds, a treatment first applied to combat casualties in the form of Sulfamylon Burn Cream in December 1967. “The Army Burn Center and the U.S. Air Force collaborated to develop a system of staged intercontinental transfer of severely burned patients, which reduced in-transit mortality to the vanishing point,” he said. Rasmussen credits Dr. Basil Pruitt, an Army surgeon during the Vietnam War, “for leading advances in clinical care and new innovations in burn and critical, intensive care,” which included “spearheading the Burn Flight Team, the predecessor of today’s Critical Care Air Transport Teams.” According to a 2014 paper in Trauma Acute Care Surgery, in which Rasmussen and Pruitt compared military trauma care and research in Vietnam to that in Afghanistan, “Trauma care in Vietnam has been the prologue to today’s much-improved care, which is attributable to a volunteer surgical workforce with greater trauma and systems training, the establishment of a global Joint Trauma System, and a sizable, requirements-driven program of intramural and extramural trauma research.” Improved blood supply availability and distribution, blood storage technologies, and the predominant use of Type O (universal donor) blood for transfusion, were also important areas of improvement in combat casualty care in Vietnam. The Army established a central blood bank in Saigon by April 1965, with four depots across the country. There was widespread blood donation from military personnel, their dependents, and civilians working on military bases. As Rasmussen and Pruitt wrote in 2014: “The recent advocacy of fixed-ratio blood component therapy can be viewed as an attempt to mimic whole blood resuscitation which was available and used in Vietnam.”
Between World War II and the Korean War, important developments were made in the area of vascular surgery, where an increase in repair of blood vessels reduced the need for amputations from 49 percent to 13 percent. In some cases, Mobile Army Surgical Hospital (MASH) units were the setting for field testing of new techniques. They were also sites for training surgeons in new techniques of vascular repair—as was the case when surgeons from each MASH unit in Korea were sent to the 43rd Surgical Hospital for training by Lt. Col. Carl Hughes, M.D. By the time of the Vietnam War, surgeons had more experience in direct repair techniques than ever before. “The only people who gain from warfare are young surgeons,” said the 16th century French military surgeon Ambrose Paré, in a passage quoted by retired Col. Norman Rich, M.D. When Dr. Rich was surgery chief of the 2nd MASH in 1965-66 in An Khe performing artery repairs and other surgeries, he systematically recorded everything he saw and did. This was the beginning of the Vietnam Vascular Registry, a body of knowledge that would eventually enable physicians and patients worldwide to benefit from the experience of young surgeons in Vietnam. Upon his return from Vietnam, Dr. Rich became the vascular research coordinator at Walter Reed Army Institute of Research in 1966, then chief of the vascular surgery service at Walter Reed Army Medical Center in 1967. It was there that he formalized the Vietnam Vascular Registry, which, combining his experience with that of surgeons at other military hospitals in Vietnam, contains information on more than 7,500 patients. The registry allows for long-term follow-up on veterans who had acute vascular injuries in Vietnam. It also has provided insight into the long-term results of these operations, as well as moral support to Vietnam veterans. The VVR also has played a crucial role in research. The first formal vascular registry was created by Drs. Michael E. DeBakey and Fiorindo A. Simeone from a review of more than two thousand vascular injuries from World War II. Their paper, “Battle Injuries of the Arteries in World War II,” was published in April 1946. The current Global War on Terror Vascular Initiative is a registry begun about ten years ago. Comparisons among these and other registries have provided best-practice guidelines based on objective data, leading to the widespread adoption of improved repair techniques such as end-to-end anastomosis, vein grafts, lateral sutures, and thrombectomy. These techniques significantly reduced the rates of amputation, especially compared to the ligation commonly practiced during the Second World War. “We know from World War II statistics that if you ligate or tie off the major artery in the leg, the amputation rate was about 55 percent,” Dr. Rich said. In cases in which medical personnel in the field cannot feel a pulse, the Doppler Ultrasound can be used to help determine whether a patient’s collateral circulation is strong enough to reach the definitive surgical arena before being treated. The Doppler’s proponent for battlefield use, Dr. George Lavenson, was an Army colonel and a fellow in vascular surgery in the program that Rich established at Walter Reed in 1967.
Rasmussen said that Rich’s Vietnam Vascular Registry, along with the Wound Data Munitions Effectiveness program, also served as an “antecedent of the current Department of Defense Trauma Registry,” which assesses the wounding capacity of enemy weapons. Along with wounds from the advanced firepower used in Vietnam, Rich also treated more than 230 patients who had been wounded by punji sticks. He was impressed by the damage this simple weapon could inflict. It was just “sharpened bamboo placed at various angles on the ground or placed in various booby-trapped devices,” Rich wrote in a 2006 article in U.S. Medicine. But some “had wounds that knocked them out of their ability to perform their duty for about as much time as some of the smaller caliber missile injuries. They were very effective primitive weapons that had been used for several centuries in jungle warfare.” In the process of studying weapons and their effects, Dr. Rich found a tremendous amount of variation. When he and his colleagues tried to study why there were differences, he said, “that got us into many exchanges with weapons developers and physicists and other specialists who understood much more than we did about the flight of a missile.” Faced with the question of what constitutes “indiscriminate suffering,” he said, “I think the tragedy is that, whereas in the last two hundred years the care of the wounded on the battlefield has improved phenomenally, we haven’t learned how to quit shooting each other.”
In 1976, Dr. Norman Rich was appointed to start a surgery department at Uniformed Services University of the Health Sciences in Bethesda, Maryland. According to Rasmussen and Pruitt, USUHS “has become a central source of career military leaders in surgery and medicine.” It also trains and holds examinations for a diploma for the medical care of catastrophes, which include natural and manmade disasters, both civilian and military. Over the years, the university has held exchange programs for young surgeons from many nations, including the Philippines, Mexico, Germany, France, Russia, and Japan.
When interviewed for this article, Lough mentioned another physician, Col. Robert Hobson, who served with Special Forces in Vietnam. He, too, was deeply involved in vascular research. “Both Dr. Hobson and Dr. Rich, in addition to being gifted researchers, were also tremendous teachers of future surgeons,” he said. Dr. Lough pointed out that while the Vietnam War was “critical and pivotal to our development of the wartime capability in surgery that we have today,” not all the credit should go to the physicians and surgeons. “As for the individuals who participated in the Vietnam War and suffered injuries, their care experiences directly contributed to the superior results we have seen in the most recent conflicts, in Iraq and Afghanistan,” he said. “The lessons of those experiences were not lost, and their sacrifices did have value.” |
||||||||||||
|
|
||||||||||||
|
||||||||||||
8719 Colesville Road, Suite 100, Silver Spring. MD 20910 | www.vva.org | contact us |
||||||||||||





















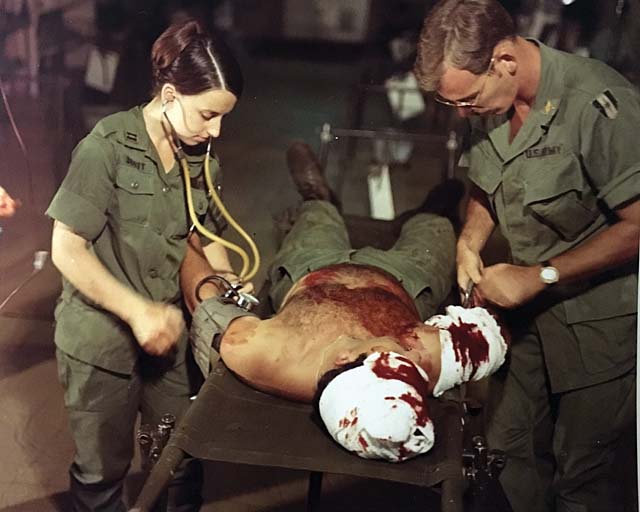

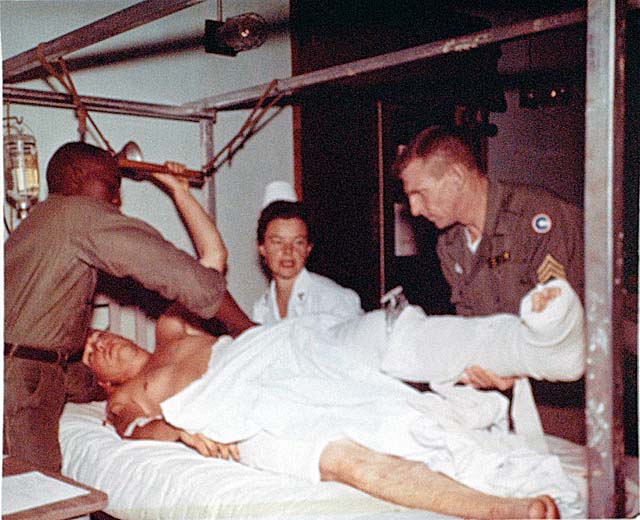
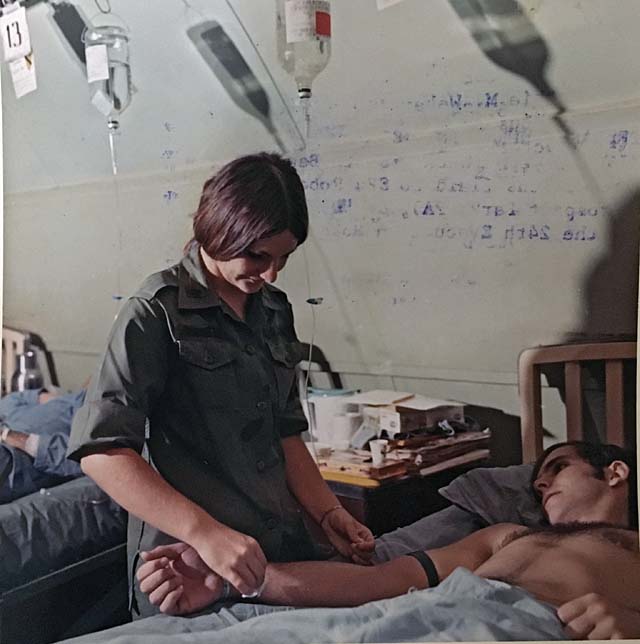 Before and during transport from the battlefield to the hospital, time is critical, but so is the quality of intervention. “The care provided those patients [in Vietnam] was, at the time, state-of-the-art in terms of mechanical ventilation, physiologic monitoring, and fluid resuscitation and achieved further reduction in mortality of casualties with penetrating and visceral injuries,” said Air Force Col. Todd E. Rasmussen, M.D.
Before and during transport from the battlefield to the hospital, time is critical, but so is the quality of intervention. “The care provided those patients [in Vietnam] was, at the time, state-of-the-art in terms of mechanical ventilation, physiologic monitoring, and fluid resuscitation and achieved further reduction in mortality of casualties with penetrating and visceral injuries,” said Air Force Col. Todd E. Rasmussen, M.D. 
 Dr. Fred Lough grew up in a military family, attended West Point, served in the Army Corps of Engineers, took Airborne and Ranger training, and in 1971 entered the George Washington University School of Medicine. After residencies at WRAMC in Washington, D.C., he embarked upon a civilian career, rising to the position of Director of Cardiac Surgery at GWU Hospital. After September 11, 2001, he enlisted in the Army Reserve and served as deputy commander of a NATO hospital in Afghanistan. More recently, he has returned to active duty as a professor on the Department of Surgery faculty at USUHS. “Being a military physician is a great way to serve, not only our wonderful soldiers, but our fellow man,” he said at his USUHS swearing-in ceremony in 2013.
Dr. Fred Lough grew up in a military family, attended West Point, served in the Army Corps of Engineers, took Airborne and Ranger training, and in 1971 entered the George Washington University School of Medicine. After residencies at WRAMC in Washington, D.C., he embarked upon a civilian career, rising to the position of Director of Cardiac Surgery at GWU Hospital. After September 11, 2001, he enlisted in the Army Reserve and served as deputy commander of a NATO hospital in Afghanistan. More recently, he has returned to active duty as a professor on the Department of Surgery faculty at USUHS. “Being a military physician is a great way to serve, not only our wonderful soldiers, but our fellow man,” he said at his USUHS swearing-in ceremony in 2013.